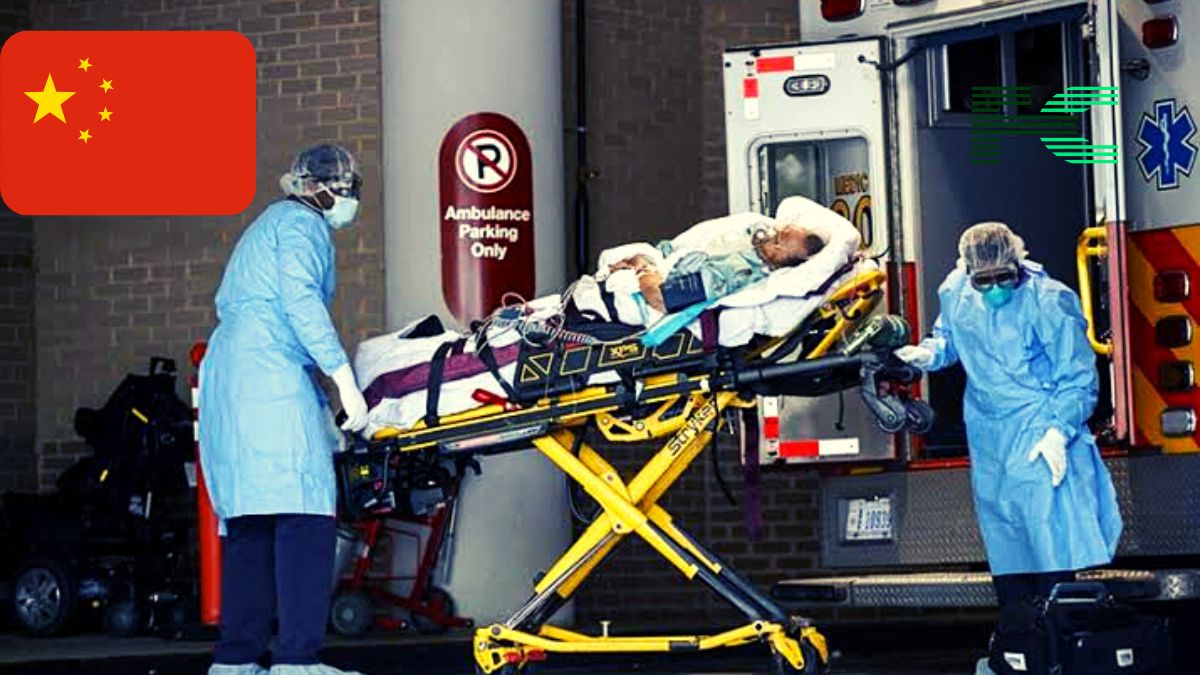
As Chinese authorities strive to alleviate the pressures of sweeping pandemic lockdowns, lengthy quarantines, and routine mass testing, the country’s hospitals are experiencing the initial shock of a massive wave of infections and a scarcity of health staff.
Since the State Council, China’s cabinet, announced a new 10-point plan on Wednesday to relax Covid-19 controls, including ending mass nucleic acid testing and allowing some infected people to quarantine at home rather than in centralized facilities, hospitals have faced increased workloads as infections have surged.
Fever clinics are full of people in places like Guangzhou, Shijiazhuang, and Beijing, which have taken the lead in implementing the new policy, and cross-infections between patients and doctors have begun to occur.
Experts foresee a spike in infections in the next one to three months, with roughly 60% of the population affected, putting a strain on already overcrowded hospital emergency departments and intensive care units and exhausting healthcare employees.
With difficulties such as a shortage of intensive care resources, a significant urban-rural gap in health resources, and still-immature telemedicine, mitigating the impact of the coming surge has emerged as China’s most pressing challenge as it continues to shift away from the stringent “zero-Covid” strategy.
In the central city of Wuhan, the core of China’s Covid-19 outbreak in early 2020, authorities issued a list of 42 fever clinics on December 1, but several of them closed only a few days later due to an excess of infected patients and employees.
One of the difficulties for healthcare providers in hospital emergency rooms and fever clinics is distinguishing Covid patients from non-Covid cases. “Some patients arrived at the hospital with normal temperatures after taking fever treatment, but later tested positive, creating cross-infection at the hospital,” said Shao Yang, an ER doctor at a Wuhan hospital.
According to the National Health Commission’s ninth version of Covid-19 diagnosis and treatment guidelines, released in March, hospitals must treat patients with suspected cases in single rooms while waiting for nucleic acid test results and place confirmed infected patients under centralized quarantine or send them to designated hospitals.
However, such interventions cannot keep up with the rising incidence of infections.