Athlete’s foot, also known as tinea pedis, is a fungal infection that develops between the toes and under the soles. “Globally, athlete’s foot affects about 15% of the population,” Wikipedia reports. This fungus doesn’t really have a preference; it will infect anyone who will allow it to enter, but it really likes to make itself at home in moist public spaces like saunas, swimming pools, and locker rooms. In this article, we’re going to look at the symptoms, causes and treatment of athlete’s feet.
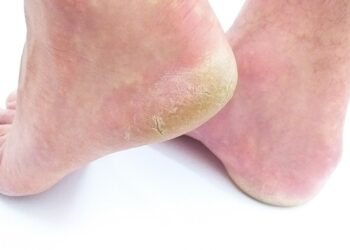
Symptoms of Athlete’s Foot
| Common Symptoms | Less Common Symptoms |
|---|---|
| Itching between the toes; scaling & flaking skin | Blisters or cracks |
| Burning sensation | Thickened soles |
| Redness and irritation | Nail discoloration |
Causes and Mode of Transmission Athlete’s Foot
The main cause of athlete’s foot, also known as tinea pedis, is fungus, most frequently different species of Trichophyton. The ideal conditions for the growth and proliferation of the fungi that cause athlete’s foot are ones that are warm and damp. Particularly if you’ve been sweating enclosed shoes and socks create a damp microclimate around your feet. Direct touch with infected skin or contact with surfaces contaminated by the fungus are the two ways that athlete’s foot spreads. This can occur while using infected shoes, socks, or towels that have been worn by someone who has the infection, or when going barefoot in public areas like locker / changing rooms. The fungus can last on surfaces for a long time while it waits for its next unwitting host to come into contact with it.
Risk Factor of Athlete’s Foot
Frequent Sweating: People who sweat excessively, whether via physical activity or living in warm climates, are at a higher risk. The moisture from sweat creates a great environment for the fungus to grow.
Wearing Tight-Fitting or Non-breathable Shoes: Shoes that are too tight or composed of materials such as nylon trap moisture and warmth, providing a comfortable environment for fungi. This promotes the infection’s spread.
Personal Objects: Sharing personal objects such as towels or shoes increases the danger of the fungus spreading from one person to another.
Weakened Immune System: A weakened immune system, whether due to disease or medicine, makes it more difficult for the body to fight fungal infections, increasing the risk of athlete’s foot. Also certain medical problems, such as diabetes, can impair circulation and nerve activity in the feet, making people more susceptible to infections like athlete’s foot and taking longer to recover from them.
Treatment of Athlete’s Foot
Over-the-Counter Medication: In the majority of cases of athlete’s foot, over-the-counter antifungal drugs are the first line of defense. These medicines come in a variety of forms, including creams, sprays, and powders, and they operate by destroying the fungus that causes the infection. They are widely available in pharmacies without a prescription and are effective in mild to moderate instances.
Prescription Oral Medication for Severe Cases: If the infection is severe or does not respond to topical therapy, a healthcare professional may recommend oral antifungal medication. These drugs battle fungal infections from the inside out. They are often used for more obstinate or widespread instances of athlete’s foot and may necessitate a doctor’s examination and prescription.
Home Remedies: Some people use home remedies to treat athlete’s foot, such as bathing their feet in vinegar or applying tea tree oil.
Conclusion
In conclusion, athlete’s foot, or tinea pedis, is a common fungal infection that flourishes in warm, damp settings. It can cause itching, scaling, redness, and irritation, as well as consequences including blisters or nail involvement. Sweating, wearing tight-fitting shoes, sharing personal goods, compromised immune systems, and certain medical disorders, such as diabetes, are also risk factors. Treatment typically consists of over-the-counter antifungal drugs, with prescription choices available in severe cases.